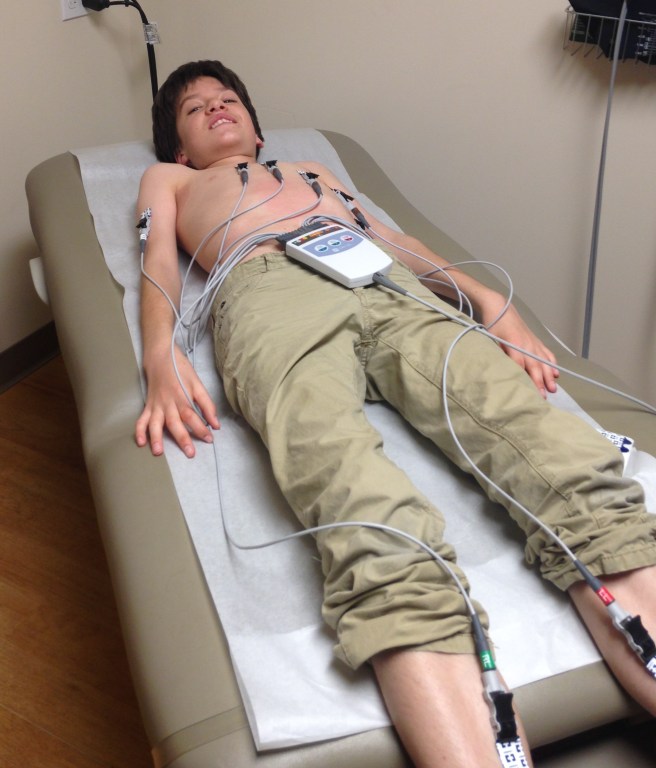
Our week was filled with the tests and medical appointments required for surgery. A visit to the pediatrician for an EKG and medical clearance. An appointment over the hill for a pulmonary exam and spirometer (lung capacity) test. A trip to the local hospital for a series of xrays (just one month after the last set) and another to the lab for urine and blood tests. By the end of the week I was fried. I’d grown weary of speaking in vague terms so as not to ignite Oscar’s anxiety and unleash a torrent of questions.
At the pediatrician he learned that he won’t be eating solid food for the first couple of days after surgery. A typical kid might shrug this off, but it’s different with a kid with Prader-Willi syndrome. “What do you mean I won’t be eating!? How will I get the food I need?” These are questions I can answer deftly when we have time. In the car on the way home or even in the parking lot, but Oscar’s anxiety and rigidity mean that he wants answers right then, in the doctor’s office, when I’m in the middle of asking how much to increase the Miralax prior to surgery so we know he’s going in with a cleared gastrointestinal system instead of the usual backed-up situation. Or when I’m trying to determine whether the medication he needs to take for the week prior to surgery comes in liquid form. (He can’t swallow horse pills, and no this is not the time to undertake that project with a kid who can’t even use his tongue to move food to the sides of his mouth for chewing). His questions, valid and well-intentioned, take extra time to be articulated and then with his processing speed, anxiety, and learning challenges he’s slower to comprehend the response. He’s not happy with the simple answer. He doesn’t quiet when I say “let’s chat in the car.” He just keeps talking. He can’t help it. I know that. But still I get frustrated.
Heading into the pediatrician’s office on Tuesday we practiced strategies for when he wanted to talk. “Tug on your ear once,” I said, “and I’ll know you have a question. But don’t interrupt the doctor.” That worked for his first two questions but when it got to the question of food, he couldn’t help himself. His voice rose, his speech quickened. He was worried. This surgery was rocking his foundation — the thing we work so hard to build — food security: the knowledge that he will get the right amount of food for his body at the right times. He doesn’t get choices, he doesn’t get to ask for more, but he will, always, get what he needs. He relies on this…it’s what gets him through what most people with PWS experience…a constant lack of satiety. No matter how much food he eats he could always eat more. He would always want more. So to learn that he won’t get to eat was highly concerning.
I didn’t handle this elegantly. I reminded him of our ear tug plan. But then I just stuck up my hand. “Stop,” I said, over and over. “We’ll talk about it in the car.”
It’s all going to work out,” I added. Softer this time.
Just not sure who I was talking to…him, or me?
